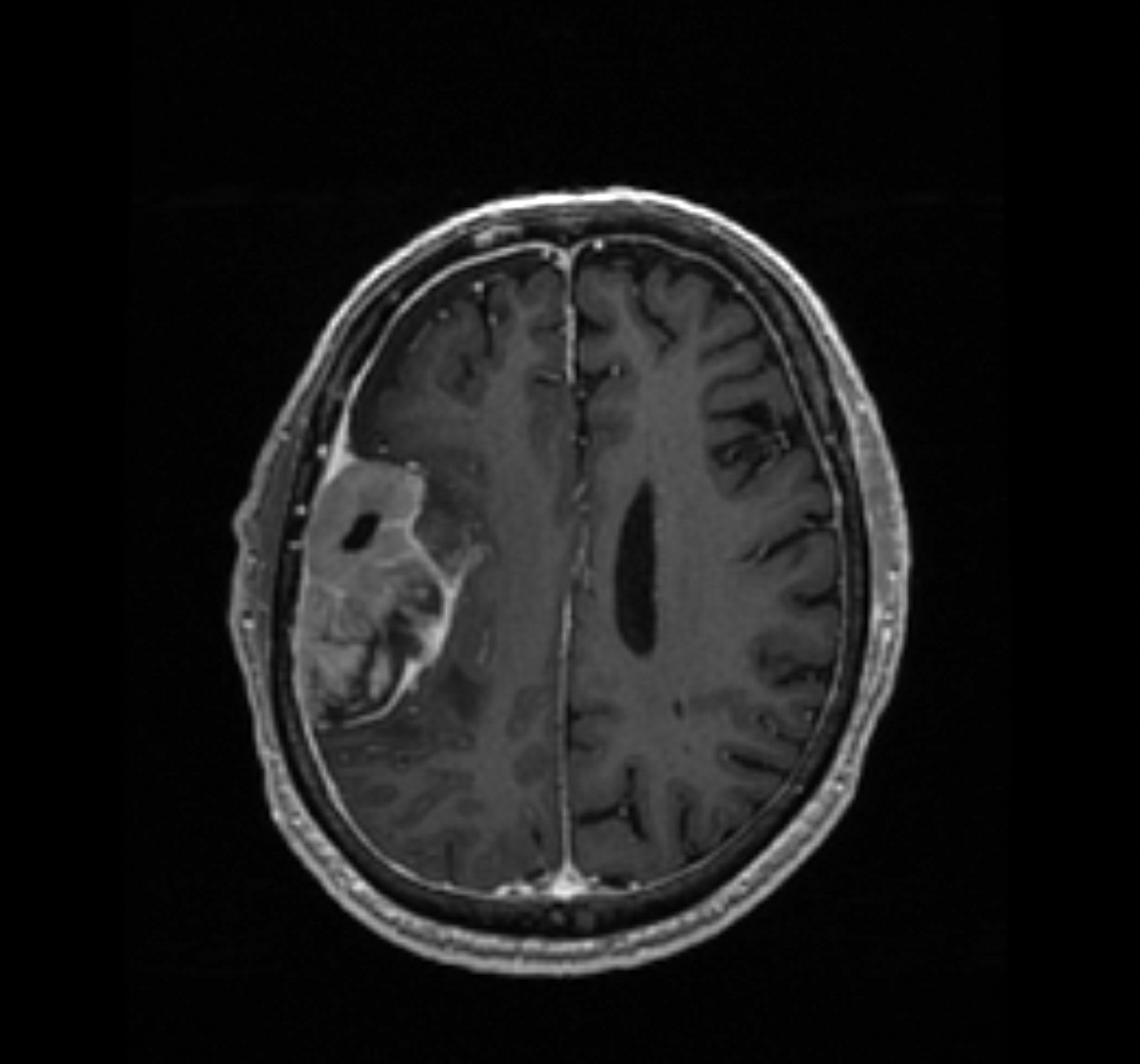
Pinpointing the origins of treatment resistance in meningioma
New UCSF study identifies a potential meningioma drug target
By Alejandra Canales
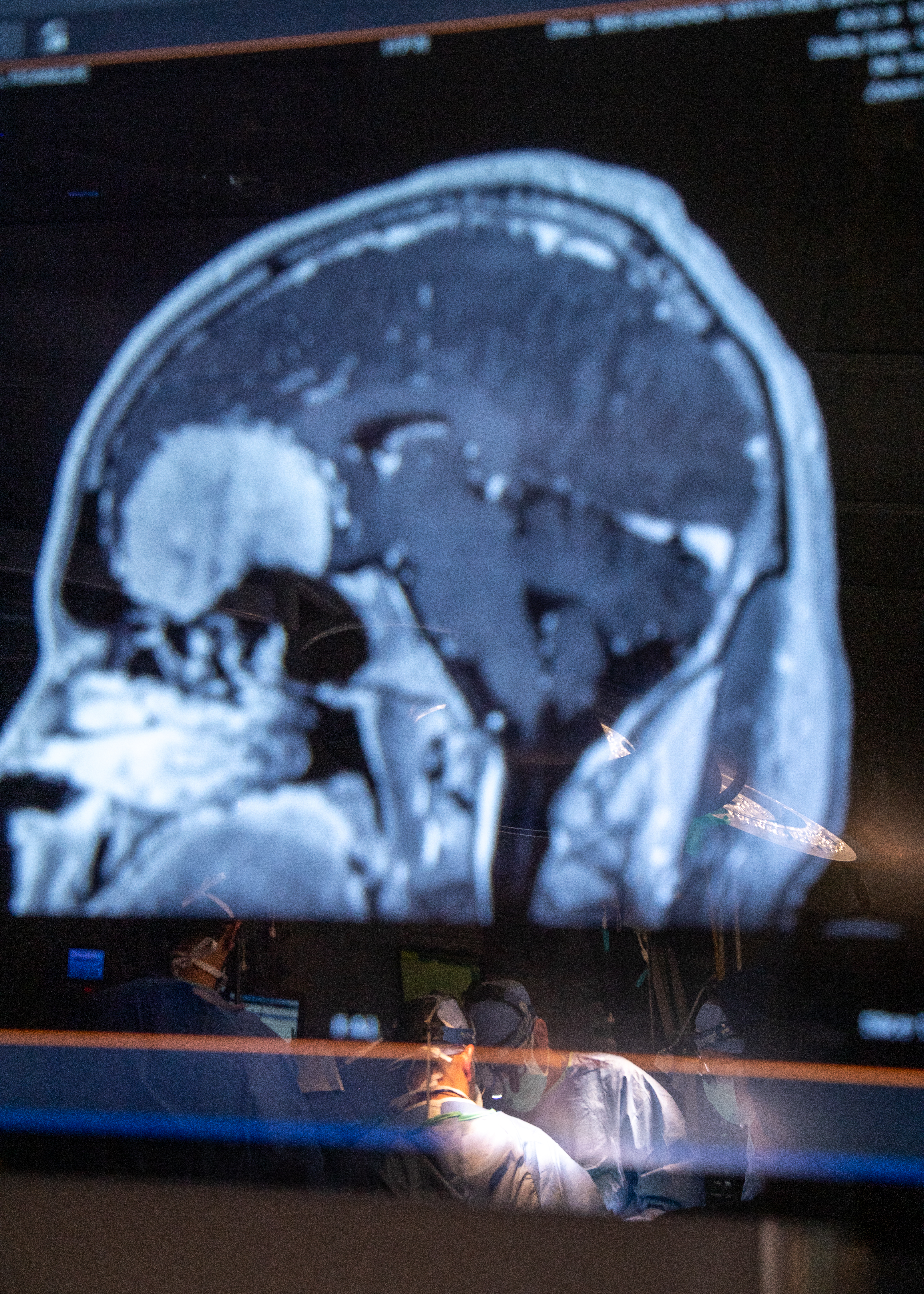
High-grade meningiomas remain difficult to treat because they are often resistant to radiation — the only other currently available option aside from surgery.
But researchers at UC San Francisco have now uncovered how these brain tumors evolve and the biology driving their resistance to radiotherapy.
Their findings in preclinical models, published on May 14 in Cancer Discovery, indicate that an antibody blocking the activity of a signaling protein called NOTCH3 could be a potential therapeutic strategy for managing tumors that do not respond to standard-of-care treatments.

“We know what tissues these tumors come from, but we didn’t really have a good idea of which cells within those tissues give rise to what can be very large tumors – nor how to specifically target them,” said David Raleigh, MD, PhD, a physician-scientist at the UCSF Brain Tumor Center and the study’s senior author.
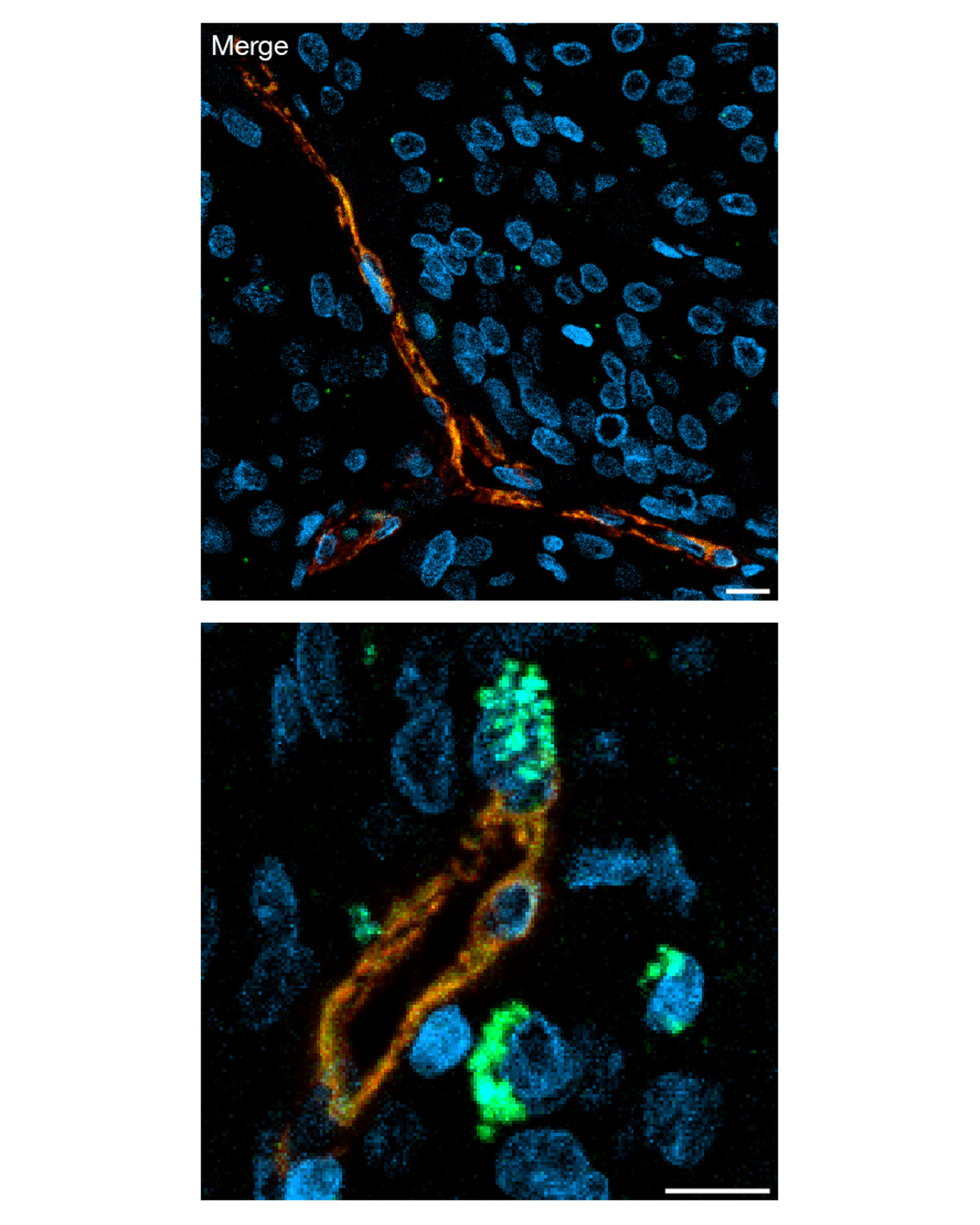
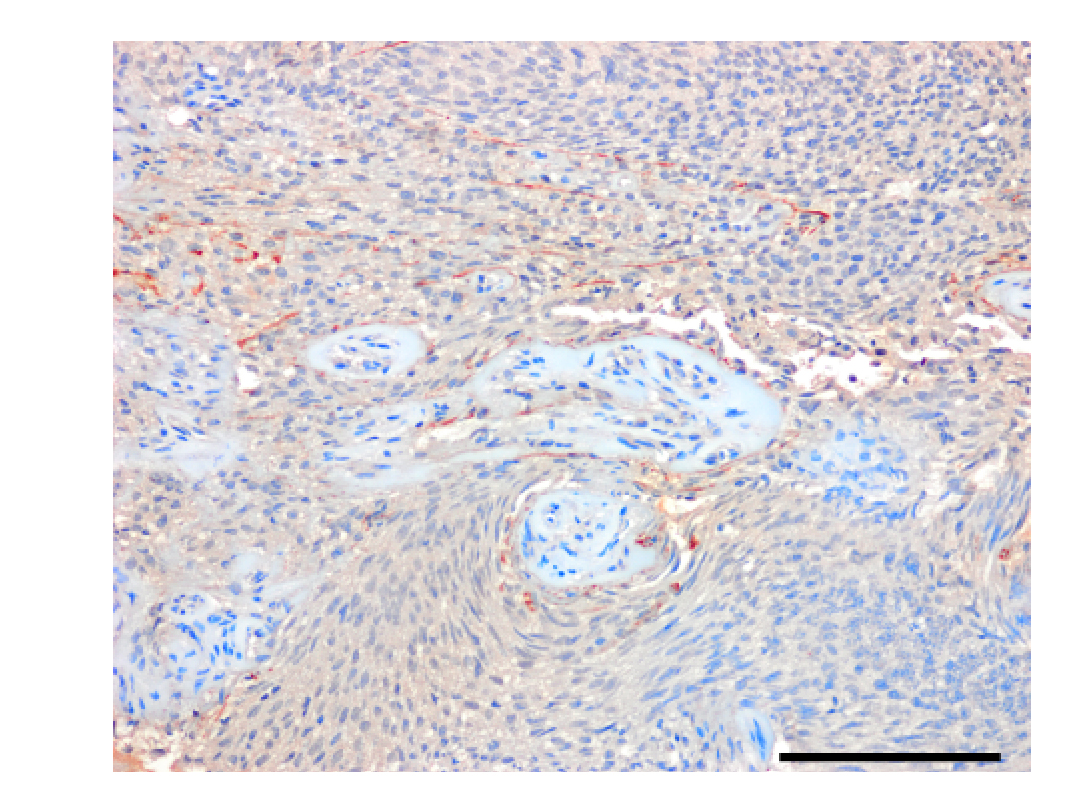
He and his colleagues found that mural cells, which supply the tumor with the blood flow necessary to promote its growth, play an important role in driving tumor formation. The scientists could distinguish these cells from the other tumors cells based on the presence of the NOTCH3 receptor protein.
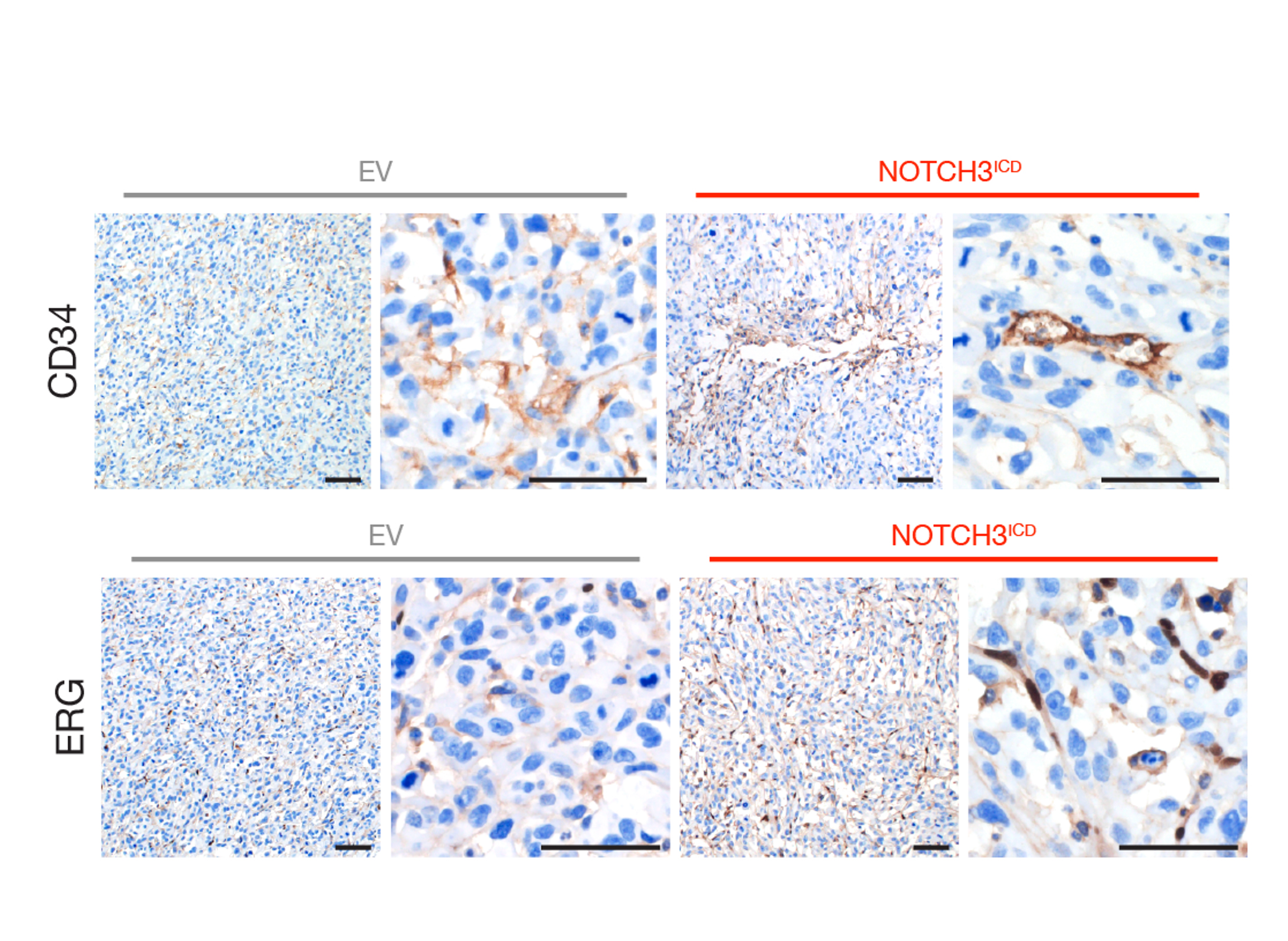
Scientists know that this protein is important in cerebrovascular disease and in other types of cancers. In this new study, Raleigh’s lab shows that the NOTCH3 protein helps the developing meningioma communicate with other tumor cells to grow and form new blood vessels.
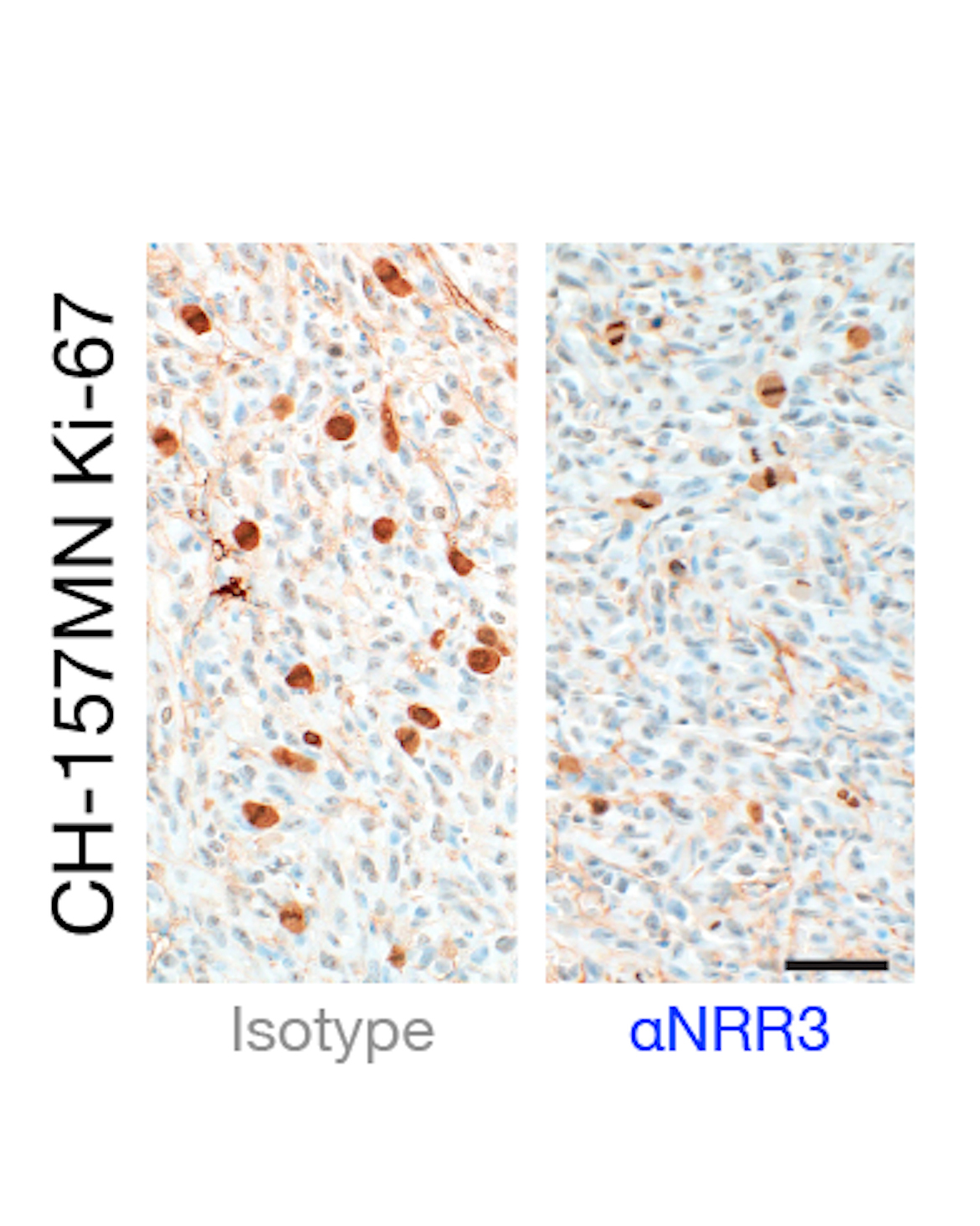
“In preclinical models, we show that we can target the biology that’s found in these cells to block the growth of these tumors and overcome radiation resistance,” Raleigh added.
Researchers have been interested in how this protein contributes to cancer growth for decades, but he says that previous attempts to block its activity with a small molecule inhibitor were too nonspecific.
“With selective targeting of NOTCH3 signaling receptors, we might overcome some of the toxicities of previous attempts to block this pathway,” Raleigh said.

He and his colleagues are now working to bring this technology into the clinic. Working with UCSF neuro-oncologist Nancy Ann Oberheim Bush, MD, PhD, they are in the process developing a clinical trial at the UCSF Brain Tumor Center for meningioma patients based on this data.