
Aggressive Brain Tumor Surgery Extends Survival Across Glioma Subtypes
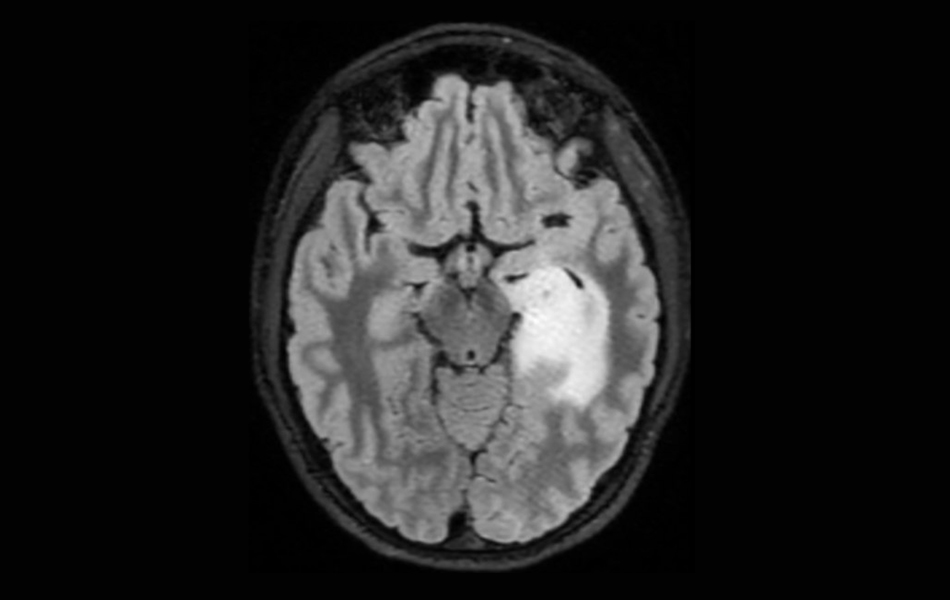
International multicenter study confirms the benefit of a greater extent of resection in patients with low-grade gliomas
Maximizing the amount of tumor removed during surgery has been consistently shown to improve outcomes for patients with aggressive brain cancer. But for patients with slow-growing gliomas, who can live for decades after their initial diagnosis, the results have been harder to assess.
Now, an international study shows that adult patients with grade 2 gliomas can live longer if their surgeon performs a supramaximal resection, removing as much of the tumor as possible and beyond the margins visible on MRI scans.
The findings, led by a team of researchers from 16 institutions across the U.S., Europe, and Asia, including UC San Francisco, were recently published in The Lancet Oncology.
“This builds on the framework from our previous work that first described the benefits of extended or supramaximal resection for patients with low-grade gliomas,” Jacob Young, a UCSF neurosurgeon and one of the study’s co-authors, said.
In that 2023 study — led by Mitchel Berger, MD, the director of the UCSF Brain Tumor Center, Shawn Hervey-Jumper, MD, the Mitchel Berger Endowed Professor of Neurosurgery, and Annette Molinaro, PhD, the director of the Division of Biomedical Statistics and Informatics for the UCSF Department of Neurological Surgery — researchers demonstrated that more extensive surgery corresponded with longer overall survival in all patients with grade 2 IDH-mutant gliomas. But even in that cohort of nearly 400 patients across three hospitals, the scientists found it difficult to tease out the impact of supramaximal resection, particularly in patients with oligodendrogliomas.
The new research is the latest effort from the large, multicenter consortium known as the Response Assessment in Neuro-Oncology (RANO) resect group, which has sought to build a much larger, retrospective database to inform surgical decision-making. As a high-volume surgical center, UCSF has been part of the group since it formed in 2021.
“There has been a lot of work from the RANO resect group describing optimal surgical strategies for patients with glioblastoma,” Young said. “This is the group’s first foray into the IDH-mutant glioma population.”
By tracking the outcomes of 1391 patients from 1993 to 2024, the RANO resect group was able to develop a system with four risk categories to classify the extent of tumor resection based on the volume of residual tumor left after surgery. Supramaximal resections were associated with better patient outcomes than maximal, submaximal, and minimal resections. This new classification system was then validated in an external cohort of 381 UCSF patients.
“Even different surgeons within the same institution can have slightly different practices,” Young said. “Having findings from a consortium that spans multiple continents improves the generalizability of the results.”
He also notes that, since this data was collected before IDH inhibitors became approved for treatment, the study may help frame the natural history of the disease after various degrees of resection.
The analysis also provides more evidence that, even with the expanding role of molecular testing in the management of gliomas, safely maximizing the amount of tumor resected remains an important part of the treatment strategy.
“I think one of the hardest questions for all surgeons to answer is when to conclude the resection,” Young said. “This data suggests that a supramaximal resection will improve overall outcomes for all patients with an IDH-mutant grade 2 diffuse glioma.”
Determining whether it’s safe to continue pursuing a more extensive resection, he says, is a multifactorial assessment based on conversations with the patient before surgery and the neurophysiological data from brain mapping. Surgeons are continually monitoring and mapping the brain during surgery to minimize the risk of a neurological deficit.
Young says that, through RANO and other consortia, researchers are also interested in collecting high-quality data on quality of life and other measures of cognitive performance to get a more complete picture of the long-term outcomes for these patients.
And new technologies, like intraoperative tissue assessments, intraoperative imaging, and artificial intelligence tools, he added, might also provide real-time feedback during surgery to improve risk modeling and aid decision-making.
Reference: Karschnia P, Young JS, Wijnenga MMJ, et al. A prognostic classification system for extent of resection in IDH-mutant grade 2 glioma: an international, multicentre, retrospective cohort study with external validation by the RANO resect group. Lancet Oncol. 2025;26(12):1638-1650. doi:10.1016/S1470-2045(25)00534-0