Meningiomas are associated with some birth control
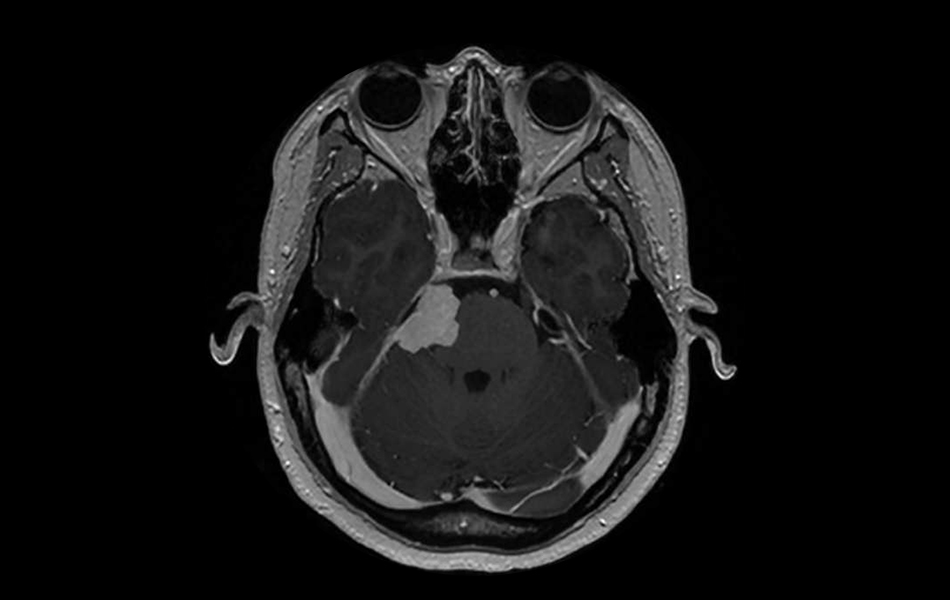
Brain tumor risk linked to progestin-based shot is lower than other birth control risks, like blood clots and stroke.
Several recent studies point to an increased risk that women have of developing a meningioma when using injectable birth control. But only a total of about 50,000 people in the U.S. are diagnosed with this type of brain tumor each year.
“While this is certainly the most common brain tumor, brain tumors aren’t all that common to begin with,” said David Raleigh, MD, PhD, a UC San Francisco physician-scientist, director of the UCSF Translational Meningioma Program, and principal investigator at the UCSF Brain Tumor Center. “The absolute risk of developing a meningioma is still very low.”
Meningiomas are two- to three-times as common in women as in men. These tumors have receptors on the surface of their cells that bind to progesterone, one of the female sex hormones. When the progesterone binds to the cancer cells, it triggers the cells to grow and form tumors.
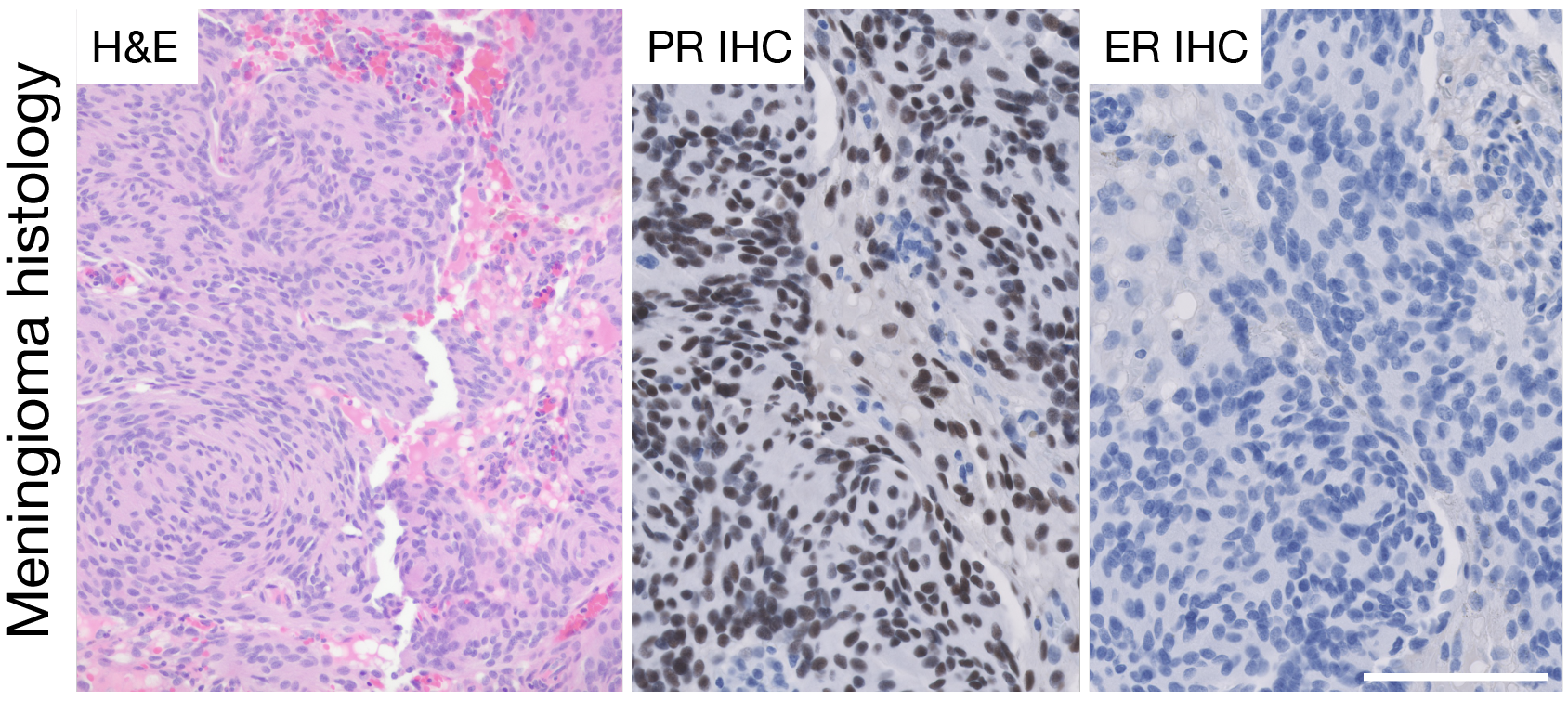
While progesterone doesn’t appear to cause meningeal cells to develop oncogenic mutations in the first place, it helps mutated cells grow. “Oncogenic meningeal cells may not be any more common in women than in men, but women just have lots more fuel to throw onto the fire to drive the growth of those transformed cells,” Raleigh said. The progesterone dose in some hormonal birth control can add even more fuel.
The birth control injection contains a synthetic progesterone (or progestin) called depot medroxyprogesterone acetate (DMPA). The new research — which includes a 2024 study in a French population, a 2025 U.S.-based study, and a 2025 Swedish study — indicates that women who used birth control containing DMPA have between a two- to six-times greater risk of developing a meningioma than those who didn’t.
“It’s a significantly elevated risk that is robust across continents,” Raleigh said.
The recent work also fits with other research that associated another progestin medication called cyproterone acetate with a higher, dose-dependent increased risk of developing meningiomas. This drug is not available in the U.S. but was previously more widely used in Europe as a treatment option for menopause, excess hair growth, and birth control in women, or prostate cancer in men.
Putting new risks in context
Physicians, like Jennifer Kerns, MD, MPH, a UCSF obstetrician-gynecologist, have plenty of experience with weighing the risks against the well-established benefits of birth control in their practice.
Hormonal birth control methods fall into two main categories: those that contain both estrogen and progestin and those with only progestin. The new studies largely pertain to the progestin-based birth control shot, finding no or weaker associations with other birth control options and meningioma.
Both Kerns and Raleigh are quick to point out that, in absolute numbers, approximately five in 10,000 women using DMPA for longer than a year could develop a meningioma compared to approximately one in 10,000 women not using this form of birth control.
“Evidence from well-designed studies does support an increased risk of meningioma among DMPA users; however, absolute risk remains quite low,” Kerns said. “In the absence of a known meningioma, patients should feel comfortable choosing the birth control method that best suits their lives.”
As a point of comparison, forms of birth control that contain estrogen, like the pill and the patch, can increase the risk of developing a blood clot. Although the relative risk is higher among users of estrogen-containing birth control, the absolute risk is low — about 10 in 10,000 according to the Centers for Disease Control and Prevention.
Still, blood clots can be life-threatening. Clinicians engage patients in a discussion of risks and benefits, especially those who have other underlying factors that already put them at an increased risk of developing blood clots or cardiovascular disease, and depending on the level of risk, may even advise against using combined hormonal contraceptives. Instead, these patients may want to consider a different option for birth control.
There’s always a balancing act in considering the alternatives, says Kerns, especially if a specific method is working well for someone who does not wish to get pregnant.
“We also know that we’re mitigating the many, well-known risks that are associated with pregnancy,” Kerns said. In fact, being pregnant puts an individual at a higher risk of developing high blood pressure and blood clots. Meningiomas themselves can also grow during pregnancy, when progesterone levels rise, Raleigh points out.
And although most meningiomas are low-grade, nonmalignant tumors that do not grow back after treatment, these brain tumors are a serious condition. Patients can experience changes in their cognitive abilities, personality, or neurological function because of the tumor itself or from treatment with surgery or radiation.
For Raleigh, the clinical and epidemiological data linking high doses of progestin and meningioma growth are robust. In his practice as a radiation oncologist treating patients with these tumors, he sees very little downside to informing patients about these risks.
He also notes that a similar relative increase in the risk of endometrial cancer arising in the setting of hormone replacement therapy containing estrogen only was enough for physicians to recommend against using this type of treatment approach.
“All things being equal, there’s a solid argument to be made for finding alternative means of achieving contraception and the goals of hormone replacement therapy,” Raleigh said.
Ultimately, these are nuanced discussions between patients and their healthcare providers, says Kerns, especially since each person may assess the same information about risk differently.
“That's the beauty of having these conversations with people: they get to forge their own path and decide what feels right and what doesn't feel right,” Kerns said. “We want to find the safest method for the patient, and we also want to find the method that the patient wants to use and works with their entire value system and lifestyle.”
Have more questions about the birth control shot and meningioma risk? Send us your questions and we'll answer them in a special webinar this spring dedicated to this topic.