
Surgical Simulation Lab Drives Innovation for Skull Base and Cerebrovascular Disorders
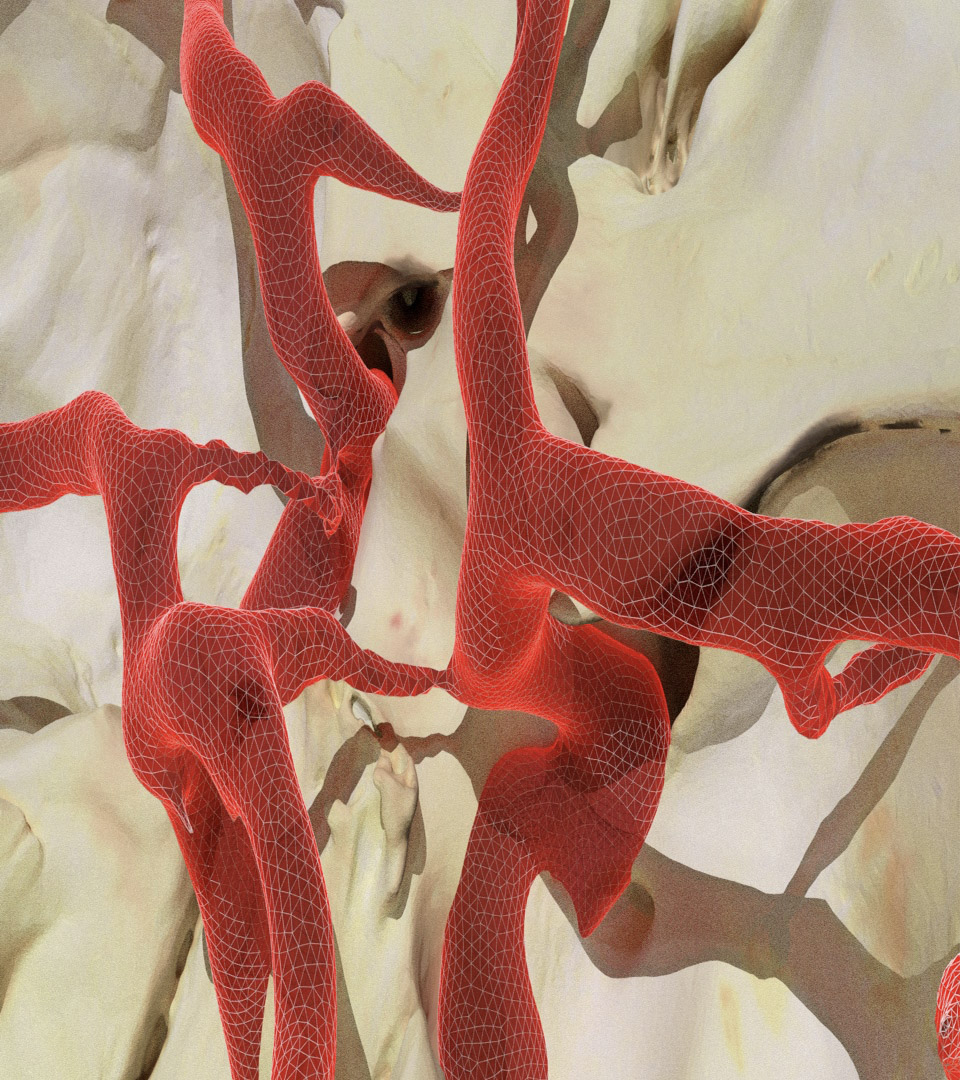
Skull base and cerebrovascular surgery are ranked among the most difficult of the surgical subspecialties. Neurosurgeons must create corridors through tiny spaces between nerves, arteries and bone to access tumors and vascular lesions. Successfully navigating these critical structures requires a masterful grasp of neuroanatomy.
“As a surgeon you cannot always rely on technology,” says Roberto Rodriguez Rubio, MD, director of UCSF’s Skull Base and Cerebrovascular Laboratory (SBCVL). “If you do, you might miss something that could result in a neurological deficit for your patient.”
In creating new anatomical models and surgical simulations, the SBCVL is currently at the forefront of developing minimally invasive routes to complex disorders and creating an entirely new way for students, residents and faculty to experience the relationship between different structures in the brain.

“Surgical simulation is a broad category,” explains Rodriguez Rubio. “Many of the models we create use donors [cadaveric models], but we also create simulations with virtual reality, augmented reality, 3D printed models and holographic display.”
Clinical Innovation
Neurosurgeons and otolaryngologists at the SBCVL are continually exploring new corridors that provide better exposure and less risk of injury. Perhaps nowhere has this exploration yielded more clinical applications than in the relatively new field of minimally invasive skull base surgery, which involves the use of an endoscope to navigate tiny corridors through the nasal passages and sinuses.
At UCSF Medical Center, head and neck surgeons and neurosurgeons often operate together on the same patient, combining expertise on navigating both the sinuses and brain tissue. In the past, many lesions of the skull base were considered inoperable or could only be accessed through large, transfacial operations that left patients with significant disfigurement and morbidity. But over the last decade routes through the endonasal corridor to the clivus, infratemporal fossa, foramen magnum, paranasal sinuses, and intracranial lesions have all been described.
In the realm of cerebrovascular disorders, Adib Abla, MD, chief of vascular neurosurgery, describes how anatomic dissections are revealing less invasive exposures for high-risk procedures that would usually need large incisions.
“Right now in the lab we are looking at how to perform a V3 vertebral artery bypass with a common carotid artery donor,” he says. “This has not previously been characterized and could be a safer way to achieve the same good outcome.”
The rules regarding surgery in eloquent regions of the brain are also evolving through research at the SBCVL. Rodriguez Rubio’s detailed models of white matter anatomy aim to identify landmarks for functional and anatomical correlation.
“Broca’s area has been described for over 150 years and we used to completely avoid eloquent areas,” says Rodriguez Rubio. “But now we have transopercular approaches to gliomas, which previously would have been prohibited. Using brain mapping, we are creating these small windows that you can approach them through safely.”
By having a realistic model to try new techniques on, surgeons at the SBCVL can rapidly receive feedback on the result of any maneuver. “The laboratory is like a time machine,” says Rodriguez Rubio. “I can go back and forth on the steps of a surgical technique. I can stop at step three and see what happens if I jump to step six. And then go back to see if there is a way to get to step three straight from step one. That’s how we start designing new corridors. At the end it’s not just beautiful dissections and models, but how we can apply this and make it meaningful.”
The Future of Medical Education
While faculty working in the SBCVL blaze new paths in the clinical setting, the lab has also become a valuable resource for medical students, research fellows and neurosurgery residents. Compared to flat images in a textbook, 3D models give a better sense of the actual distance between central nervous system structures. And as technologies improve and new ones become available, students can not only view the neuroanatomy more realistically, but experience and interact with it in a virtual environment.
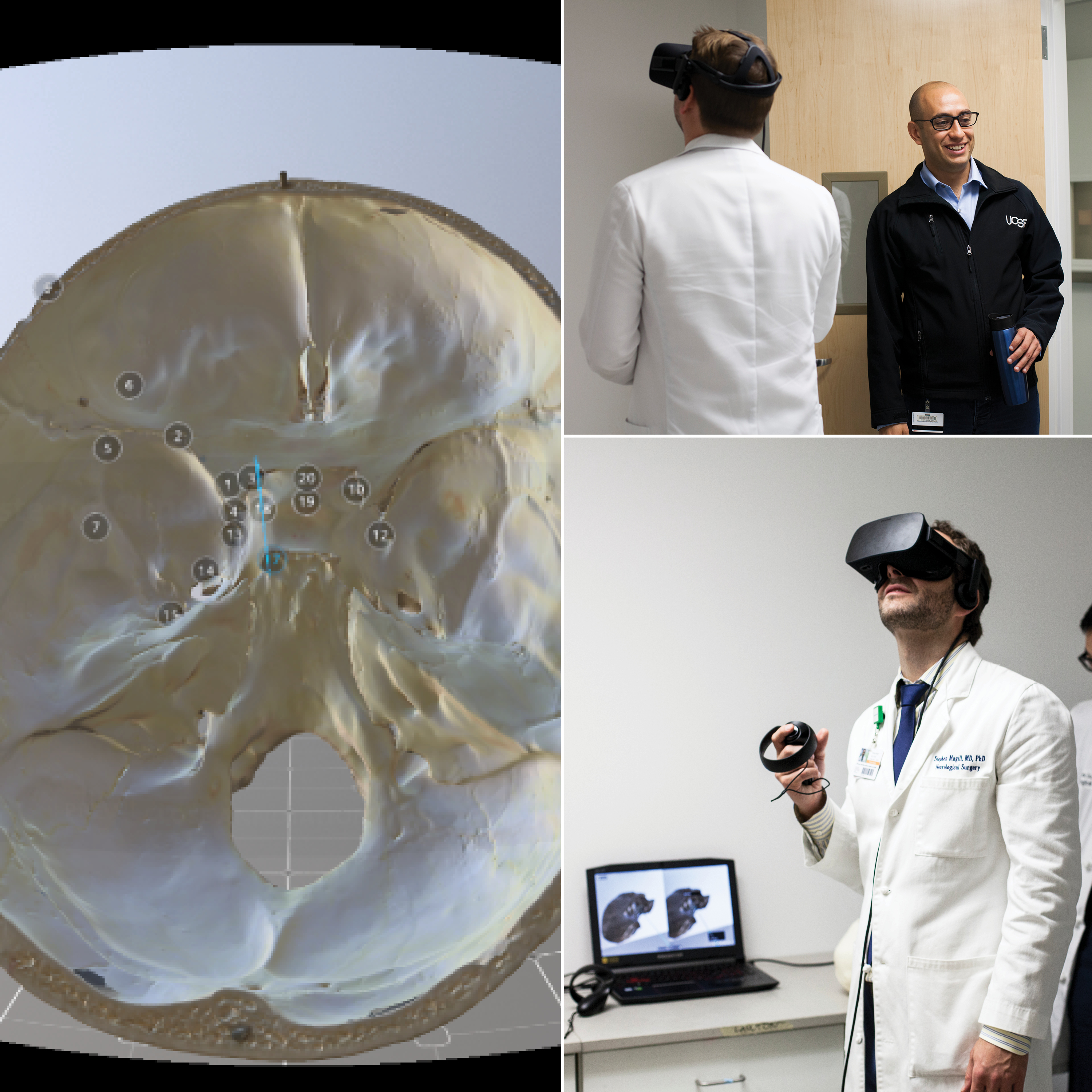
For instance, wearing virtual reality headsets, trainees and surgeons can immerse themselves in an actual patient’s anatomy, enabling them to practice the surgery ahead of time and plan the safest route. In most hospitals, a trainee may have the opportunity to practice a procedure on a cadaver once before performing it in the operating room on a real patient. With the opportunity to practice in a surgical simulation lab, they can hone their skills over more time and enter the operating room with more confidence in their ability to safely perform the procedure.
In order to recreate the environment a surgeon would encounter during a real case, the operating microscope, surgical navigation systems, and surgical instruments in the SBCVL are the same state-of-the-art models used in UCSF’s operating rooms.
The SBCVL’s dual mission of innovation and education is perhaps best embodied in its research fellowship program. To date, 33 fellows from 11 countries have graduated from the program, publishing widely on surgical techniques, neuroanatomical education practices, and modeling. By bringing their new expertise back to their home institutions, they serve as ambassadors for the program and will go on to train a new generation of surgeons and anatomists worldwide using the most advanced technologies. For Rodriguez Rubio, this is the true heart of the lab’s mission. “What is the point of this knowledge if you cannot apply it to patients and share it with others?”