
Top 5 Research Stories of 2020
In 2020, the UCSF Brain Tumor Center researchers focused on understanding meningioma biology, improving tumor resection, precision medicine therapy for pediatric glioma, and more. Here are our top five research stories of the year:
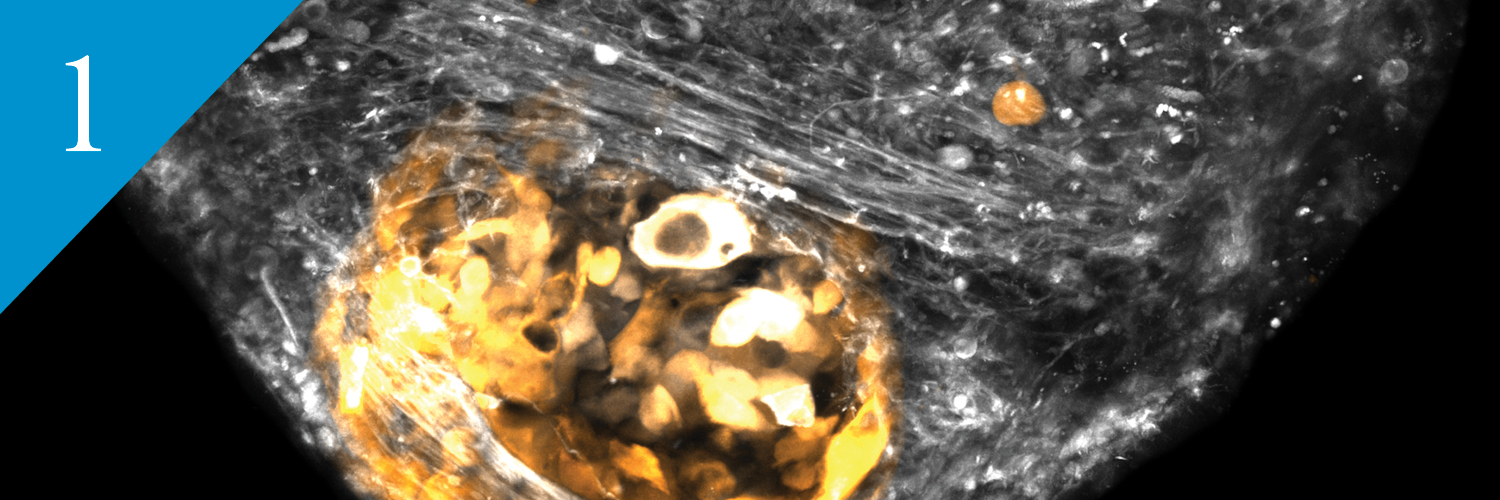
Immense Variation Found Within Meningiomas Offers Insight Into Therapeutic Targets
“Differences within tumors called intratumoral heterogeneity has increasingly been recognized as a source of resistance to cancer treatments,” said UCSF physician-scientist David Raleigh, MD, PhD. To better understand the extent of variation, or intratumoral heterogeneity, in meningioma, Raleigh and team launched a comprehensive analysis of 86 meningioma samples, collected from separate locations within 13 patients’ tumors.
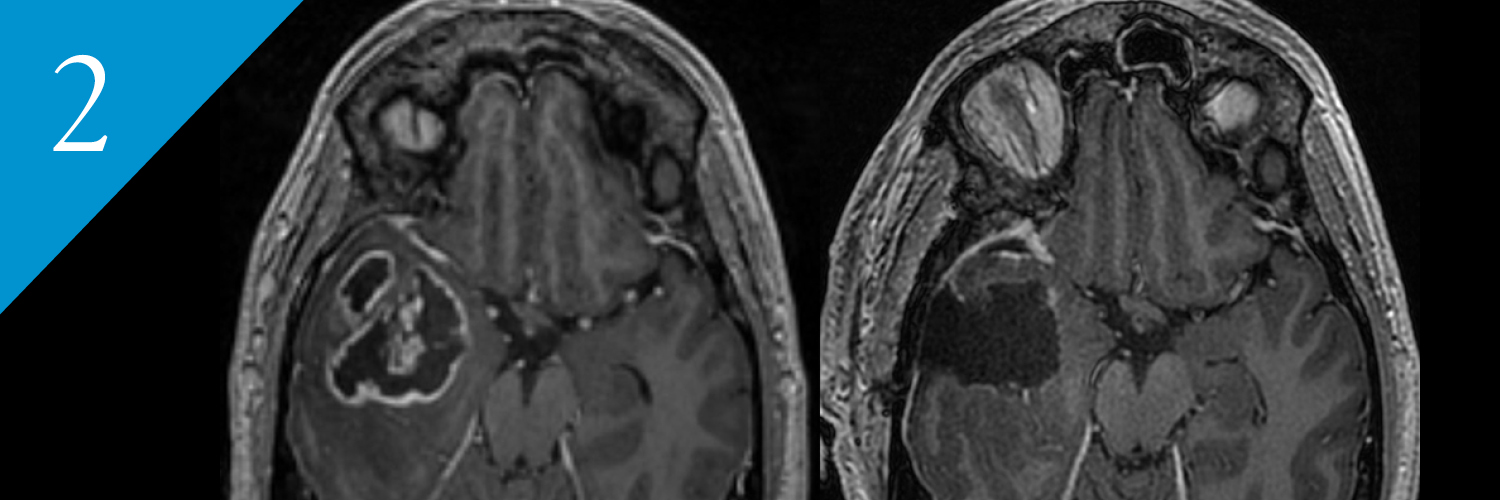
Brain Tumor Surgery that Pushes Boundaries Boosts Patients Survival
Survival may more than double for adults with glioblastoma, if neurosurgeons remove the surrounding tissue as aggressively as they remove the cancerous core of the tumor. Removing the “non-contrast enhancing tumor” represents a paradigm shift for neurosurgeons, according to senior author and neurosurgeon Mitchel Berger, MD.
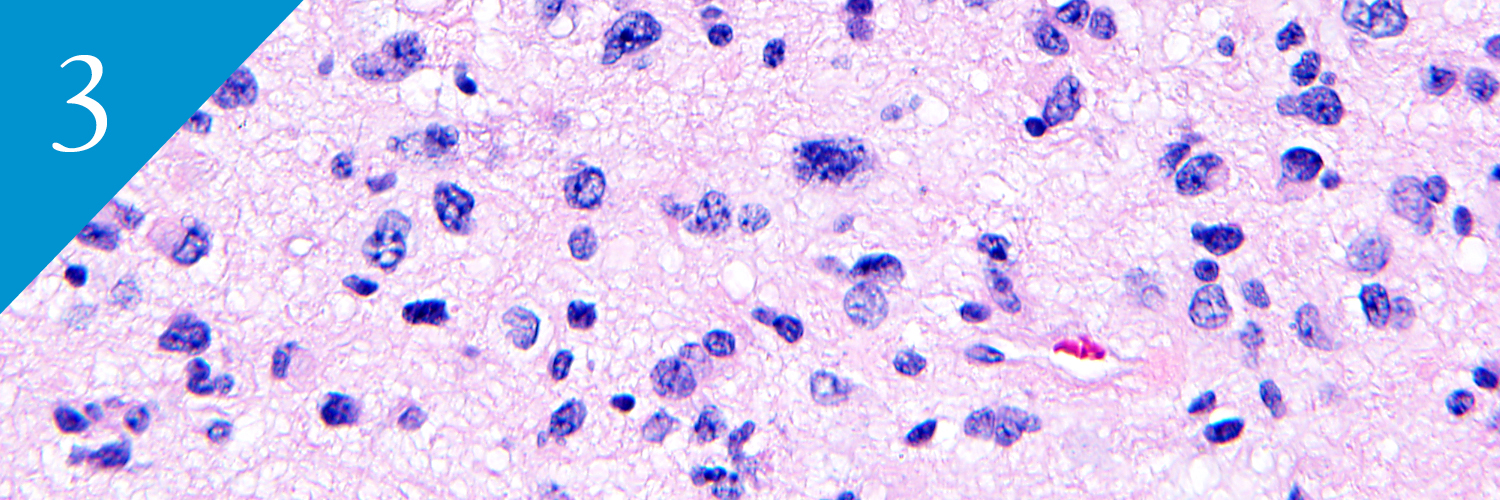
New UCSF Study Identifies Precision Medicine Therapy for Rare Pediatric Glioma
David Solomon, MD, PhD and colleagues share a comprehensive genomic and epigenomic analysis of bithalamic glioma, identifying gene alterations and a unique epigenetic signature that distinguish this rare pediatric tumor as a distinct tumor entity with potential sensitivity to a precision medicine treatment strategy.

UCSF Researchers Discover Mechanism Underlying Treatment Resistance in Glioma
Published in Cell Reports, researchers at UC San Francisco have discovered how PGAM1 – a protein expressed at high levels in many cancers – can contribute to glioma cells’ resistance to DNA damage, and thus treatments like radiation therapy and chemotherapy.
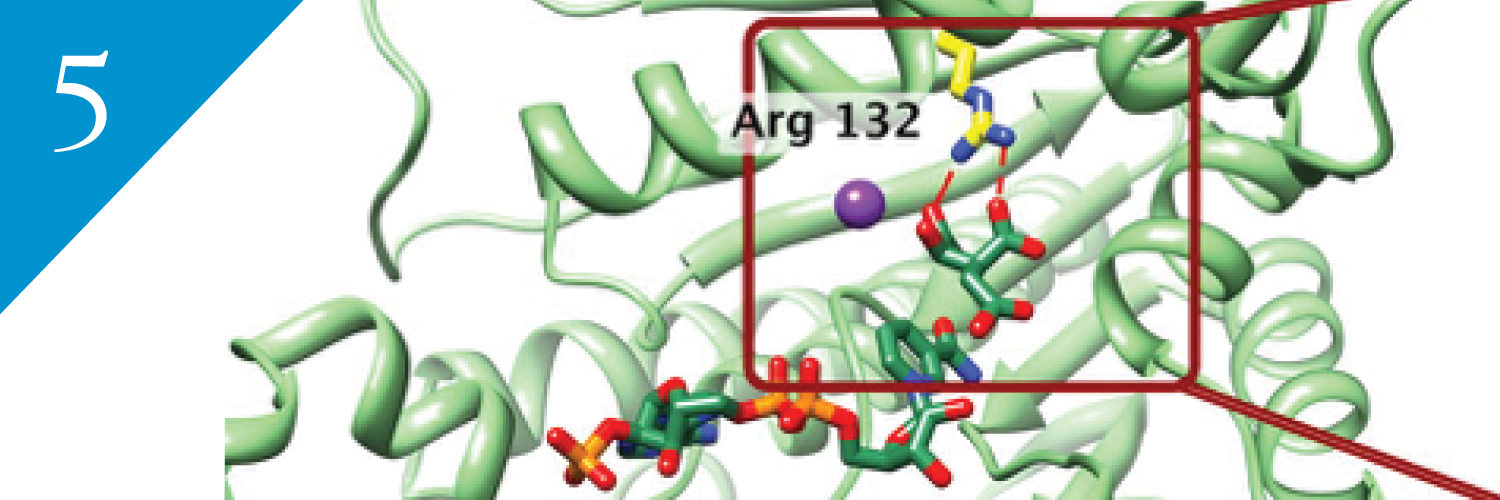
New Clinical Trial Targets Mutations Commonly Found in Lower Grade Gliomas
“With IDH mutations present in the majority of low-grade gliomas, being able to specifically target this known driver of tumor development could have enormous impact,” says UCSF neuro-oncologist Jennifer Clarke, MD, who is leading the study at UCSF.
Follow us on Instagram, Twitter, and Facebook to keep up with the latest news from the UCSF Brain Tumor Center.